HIGHLIGHTS:
Caring for your health without compromising your quality of life.
- Complete and Safe Tumor Removal: The tumor is removed with high precision and safety margins, strictly adhering to oncological criteria to ensure maximum safety and reduce the risk of recurrence.
- Full Preservation of Urinary Continence: We carefully preserve the urinary sphincter and bladder support structures, using precise reconstruction techniques that facilitate a faster recovery of urinary control. Continence rates are >95%.
- Preservation of Sexual Function: Surgery is performed with the utmost care to preserve the nerves responsible for erection, whenever clinically safe, significantly reducing the risk of sexual dysfunction after treatment.
- Superior Results with Minimally Invasive Robotic Surgery: Advanced robotic techniques result in less pain, a faster recovery, and a quicker return to your daily routine with minimal impact on your life.
- Integrated Multidisciplinary Care: A specialized team accompanies you throughout the entire journey—from preoperative preparation to post-surgical rehabilitation—ensuring you are supported at every stage of your treatment.
(Robotic Simple Prostatectomy)Treatment for Large Volume Prostates
If you suffer from significant urinary symptoms due to benign enlargement of the prostate (Benign Prostatic Hyperplasia – BPH), especially if your prostate is of a large volume, robotic prostate adenomectomy may be a highly effective treatment option.
This is a minimally invasive surgical procedure designed to remove the internal part of the prostate that causes obstruction, relieving your symptoms and improving your quality of life.
This page aims to provide clear and detailed information about this advanced surgical technique so that you can make an informed decision together with your urologist.
If you suffer from significant urinary symptoms due to benign enlargement of the prostate (Benign Prostatic Hyperplasia – BPH), especially if your prostate is of a large volume, robotic prostate adenomectomy may be a highly effective treatment option.
This is a minimally invasive surgical procedure designed to remove the internal part of the prostate that causes obstruction, relieving your symptoms and improving your quality of life.
This page aims to provide clear and detailed information about this advanced surgical technique so that you can make an informed decision together with your urologist.
1. What is the Prostate and Benign Prostatic Hyperplasia (BPH)?
The Prostate: A gland in the male reproductive system, roughly the size of a walnut, located immediately below the bladder and in front of the rectum.
The Urethra: The canal that carries urine from the bladder to the outside passes through the center of the prostate.
BPH: An enlargement that occurs naturally with aging in most men. As the inner part of the prostate (called the adenoma or transition zone) grows, it can compress the urethra, making it difficult for urine to pass and causing various Lower Urinary Tract Symptoms (LUTS).
Important Distinction: It is crucial to differentiate BPH from prostate cancer. BPH is not cancer and does not turn into cancer. However, both conditions can coexist. The tissue removed during an adenomectomy is always sent for analysis to rule out the presence of incidental cancer.
2. What is Prostate Adenomectomy (Simple Prostatectomy)?
Definition: Also known as simple prostatectomy, this procedure involves the removal (enucleation) of the enlarged internal portion of the prostate—the adenoma—that is obstructing urinary flow. The outer capsule of the prostate is left in place.
Difference from Radical Prostatectomy: In radical prostatectomy (performed for prostate cancer), the entire gland, seminal vesicles, and sometimes lymph nodes are removed. Adenomectomy is less extensive, focusing only on the obstructive benign tissue.
Difference from Transurethral Procedures (TURP, Laser, etc.): While TURP or laser therapies remove tissue through the urethra (“from the inside”), adenomectomy is generally reserved for considerably larger prostates where transurethral removal would be less effective or carry a higher risk of complications.
Main Objective: To provide significant and long-lasting relief from urinary obstruction and symptoms caused by a large-volume BPH.
3. What is the Robotic Approach?
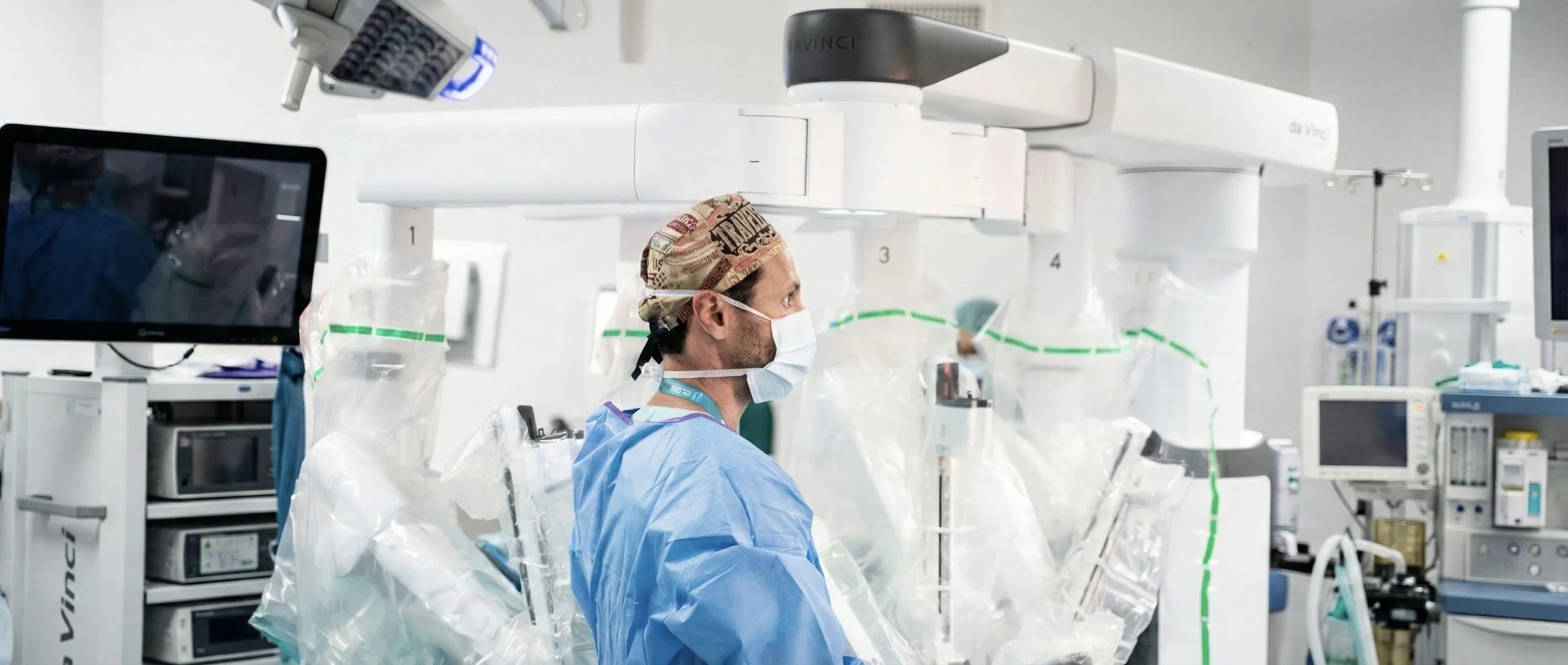
Adenomectomy can be performed via traditional open surgery or, more modernly, via the robotic route (using the Da Vinci® Surgical System).
How Robotic Surgery Works:
- It is a minimally invasive technique performed under general anesthesia.
- Several small incisions (usually 4 to 6, about 0.5 to 1.5 cm each) are made in the abdomen.
- Through these “ports,” a high-definition 3D camera and miniaturized, articulated instruments are inserted.
- The surgeon operates from an ergonomic console, controlling robotic arms that translate hand movements into precise, filtered actions inside the patient’s body.
Differences from Open Adenomectomy:
- Traditional Open Surgery: Requires a larger abdominal incision from the navel to the pubic bone. It was the standard for very large prostates before robotics.
- Robotic Surgery: Achieves the same goals of complete adenoma removal but with smaller incisions, less trauma, and faster recovery.
4. Advantages of Robotic Prostate Adenomectomy
The use of robotic technology for large prostates offers several key benefits:
Magnified 3D HD Vision: Excellent visualization of the prostate capsule, adenoma, bladder neck, and blood vessels.
Greater Precision: Articulated instruments (EndoWrist®) allow for fine movements, essential for the careful enucleation of the adenoma and suturing.
Less Blood Loss: Significantly reduced bleeding compared to traditional open surgery.
Faster Recovery: Shorter hospital stays and a quicker return to work and normal activities.
Better Aesthetic Results: Smaller, more discreet scars.
Effective for Very Large Adenomas: Successfully treats prostate volumes that would be difficult or impossible to manage adequately via transurethral routes.
5. Who is a Candidate?
Robotic adenomectomy is an excellent option for a specific group of men:
Moderate to Severe LUTS: Men who have not responded well to medical treatment.
Large Volume Prostates: Typically considered for prostates exceeding 80–100 grams.
Complications of BPH: Including recurrent urinary retention, large bladder stones, recurrent blood in the urine (hematuria), or bladder diverticula.
Adequate Physical Condition: Patients fit enough to tolerate general anesthesia and the surgical position.
6. Preparation for Surgery
Pre-Anesthesia Consultation: Evaluation by the anesthesiologist.
Pre-Operative Exams: Blood tests, EKG, etc.
Medication Adjustment: Suspending anticoagulants or antiplatelet agents as directed.
Fasting: No food or drink for several hours before the procedure.
7. The Surgical Procedure (Simplified)
Anesthesia: Performed under general anesthesia.
Access: The surgeon accesses the adenoma either through the bladder (Transvesical) or directly through the prostate capsule (Retropúbica/Transcápsular).
Enucleation: The enlarged tissue is carefully dissected and removed from within the capsule.
Hemostasis: Blood vessels are controlled with high precision.
Reconstruction: The incision in the bladder or capsule is sutured. The removed tissue is placed in an extraction bag and taken out through one of the slightly enlarged incisions.
Catheterization: A urinary catheter is placed, usually with a continuous irrigation system to prevent clot formation.
8. Post-Operative and Recovery
Hospital Stay: Typically lasts 2 to 4 days.
Urinary Catheter: Usually maintained for 5 to 7 days. You will receive instructions on how to care for it at home.
Continuous Irrigation: Used in the first hours or days to keep the bladder clear.
Activity: Physical activity should be increased gradually. Avoid heavy lifting for 4 to 6 weeks.
Hydration: Maintaining good fluid intake is essential.
9. Expected Results and Potential Side Effects
Results:
The primary goal is a marked, long-lasting improvement in urinary flow. Adenomectomy offers the highest success rates for relieving obstruction in men with very large prostates.Potential Side Effects:
- Retrograde Ejaculation (“Dry Orgasm”): This is a very common and expected effect. During orgasm, semen enters the bladder instead of exiting the urethra. It is not harmful to health but results in infertility.
- Bleeding: Lower risk with robotics, but still possible.
- Urinary Incontinence: Temporary leakage may occur after catheter removal but usually improves with time and pelvic floor exercises.
- General Risks: Like any major surgery, there are risks of infection, thrombosis, or incisional hernia.
10. Medical Follow-up
Your urologist will monitor your progress through:
Periodic consultations and symptom evaluations.
Uroflowmetry: To confirm a good functional result.
Pathology Review: Discussion of the lab results of the removed tissue.
11. My Experience with Robotic Adenomectomy
For men with BPH resulting in a very significant enlargement—generally above 80 to 100 grams—robotic adenomectomy represents the surgical approach of choice in my practice. This technique allows me to effectively remove the large volume of tissue while replicating the excellent functional results of open surgery with the benefits of modern technology. My objective is to provide maximum symptomatic relief with faster recovery, less pain, and a quicker return to normal life.
12. Final Message
If you have been told you need surgery to remove the “core” of your prostate due to its size, robotic adenomectomy may be the best path forward. I invite you to schedule a consultation to discuss your specific case and help you make the most informed decision for your health.